INTRODUCTION
Cone beam computed tomography (CBCT) is an advanced imaging modality that offers 3D exploration of the anatomical structures and a more accurate diagnosis compared to radiographies, with high clinical application in dentistry field 1,2.
The use of CBCT brings an important advantage in comparison to regular computed tomography (CT) scan, with regard to radiation exposure. CBCT exposure dose is 10 times lower than regular CT 2. Moreover, CBCT presents lower costs, easier image acquisition, fewer space requirements and interactive display modes. Despite CBCT is not recommendable for accurately represent the internal structures of soft-tissues and soft-tissues lesions, it is very applicable in dento-maxillofacial surgeries, oral implantology, image-guided endodontics and periodontics procedures 3.
In this manuscript, we show how CBCT can be used for a variety of purposes. We provide the imaging analysis of a patient who suffered a car accident and through volumetric assessment it became feasible to provide the best treatment alternative. This case report elucidates how CBCT application provide benefits to all dento-maxillofacial regions, improving diagnostic accuracy and a safer treatment planning. It is important to emphasize new studies aiming to establish safer CBCT protocols have been conducted in order to provide accuracy along with lower doses of radiation 4.
CASE PRESENTATION
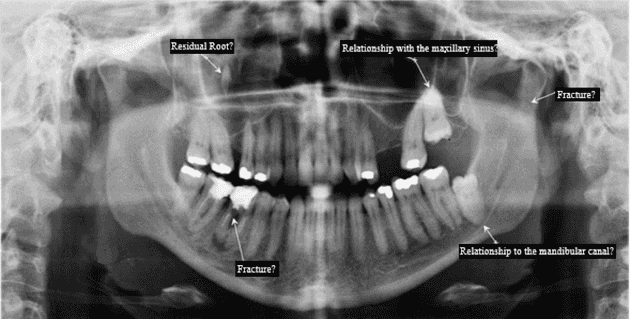
A 42-year-old female patient with aesthetic and functional impairment sought care at a dental clinic after having suffered an automobile accident. Her complaints regarded pain in the left side of the face. The panoramic radiograph (PR) showed an image suggestive of a fracture in the region of the left side mandibular ramus. However due to the excessive overlap of anatomical structures and eventual distortions in this region, which is typical of radiographies limitations 5, many questions could not be answered, reason why a CBCT was performed to complement information data.
The limitations regarding PR can be seen in Figure 1. This case demonstrates that, in more generalized cases with multiple lesions, the level of accuracy of PR is insufficient for an accurate diagnosis, being highly recommend the request of additional exams, including CBCT and MRI for brain evaluation.
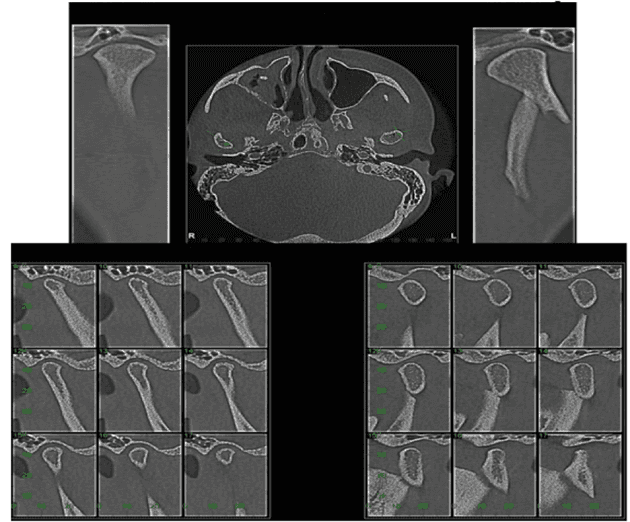
CBCT made it possible to better elucidate details in bone structures and teeth in comparison to PR image. CBCT enabled visualize a continuity condition of bone, compatible with fracture in the left temporomandibular joint (TMJ): The condyle and its relation to proximal and distal segments on fracture line, displaced from the glenoid fossa (Figure 2). The fracture line is also clearer in CBCT.
The CBCT examination showed more conclusively that the cortical structures of the bone were altered on the left side with the position of the anterior condyle in the glenoid fossa and it was possible to have a better view of the anatomy details for further treatment planning.
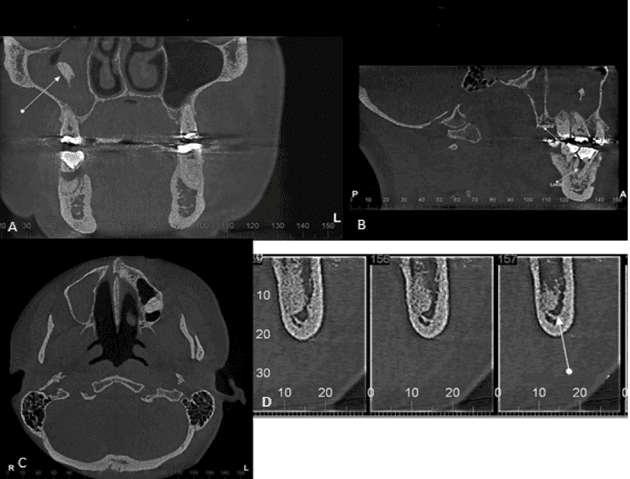
With the CBCT, it was possible to visualize the impacted tooth 28, projected in a vertical position, showing roots with extreme proximity to the floor of the left maxillary sinus (Figure 3 - Axial slice) and the roots of tooth 38 projected in vertical position with close proximity to the left mandibular canal (Figure 3 - Cross sections). Additionally, the tooth 46 presented a solution of continuity (hypodense line), compatible with a vertical oblique root fracture in the region of the cervical mesial portion of the distal root. There is a hypodense image suggestive of inflammatory odontogenic lesion (Figure 3- Sagittal section). Hyperdense material (Root fragment) lodged inside the right maxillary sinus, presenting pathological material next to de maxillary sinus walls, compatible with chronic reactional maxillary sinusopathy (Figure 3-Coronal section).
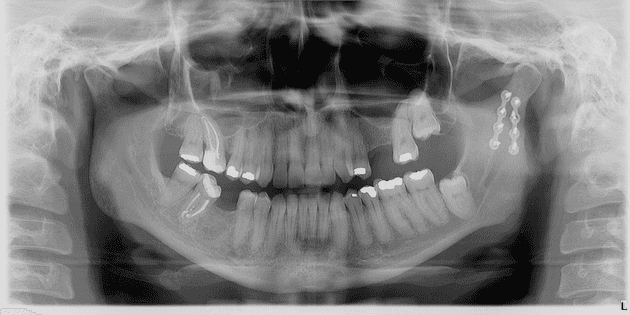
After the analysis of the complementary exams, the treatment plan could be effectively elaborated, involving the extraction of tooth 46, endodontic treatment of tooth 47 and reduction of fracture in the mandible with an internal fixation system. Subsequently, a new PR was performed showing good prognosis in the region of tooth 46 and the calcification in mandibular fracture area (Figure 4).
DISCUSSION
CBCT is a complementary imaging exam able to greatly improve the diagnostic accuracy using a lower radiation dose than conventional CT scan 1-3. Not only in the dental practice, but in pediatric otolaryngology, CBCT has been recommended as a viable alternative to CT due to its practicality and lower dose of radiation applied. CBCT has been considered a suitable imaging modality for bony structures in adults and children with settings mainly depending on the region of interest 6.
The CBCT exam is fast, taking not more than 18 seconds, which makes this procedure a good alternative for patients, such as claustrophobic or anxious people, such as children 6. In the present case report, CBCT was fundamental for an accurate diagnosis of a mandibular fracture, which was causing constant pain and was not sufficient apparent in PR so an effective treatment could be provided.
The effectiveness of the treatment in directly associated with the diagnostic capacity, and imaging techniques such as CBCT must be encouraged to better elucidate the condition of the bones and its relation to the teeth. A three-dimensional visualization of the anatomical structures provide means to assess the relation of the roots to the mandibular canal, the intrusion of foreign bodies into the maxillary sinus and to have good view of the extension of fractures that, by assessing only the PR, many questions regarding lesion extension may remain. CBCT allows for a precise evaluation and classification of bone fractures, which makes it an indispensable imaging exam in cases of accident and extensive damage to face.
Conflict of interests: The authors declare no conflict of interest.
Corresponding author
Antonione Santos Bezerra Pinto. Institute of Higher Education of Vale do Parnaíba. Rua Maria Teresa Dutra, 90, ZIP Code 64202 475. Parnaíba, Piauí, Brazil. Phone number: +55 86 99415 2880 (antonione182@hotmail.com)
REFERENCES
- Venkatesh E, Elluru SV. Cone beam computed tomography: basics and applications in dentistry. J Istamb Univ Fac Dent. 2017;51:102-121. DOI: 10.17096/jiufd.00289. eCollection 2017
- Kumar M, Shanavas M, Sidappa A, Kiran M. Cone beam computed tomography – Know its secres. J Int Oral Health. 2015;7(2):64-8.
- Kamburoglu K. Use of dentomaxilofacial cone beam computed tomography in dentistry. World J Radiol. 2015;7(6):128-30. DOI: 10.4329/wjr.v7.i6.128
- Costa ALF, Barbosa BV, Perez-Gomes JP, Calle AJM, Santamaria MP, Lopes SLPC. Influence of voxel size on the accuracy of linear measurements of the condyle in images of cone beam computed tomography: a pilot study. J Clin Exp Dent. 2018;10(9):876-82. DOI: 10.4317/jced.54500
- Turner KO. Limitations of panoramic radiography. Oral Surg Oral Med Oral Pathol. 1968;26(3):312-20. DOI: 10.1016/0030-4220(68)90401-5
- Walliczek-Dworschak U, Diogo I, Strack L, Teymoortash A, Werner JA, Güldner C. Indications of cone beam CT in head and neck imaging in children. Acta Otorhinolaryngol Ital. 2017;37(4):270-75. 10.14639/0392-100X-1219